Our Workers’ Comp Claims Advocacy promotes better communication
- Our Workers’ Comp Claims Advocacy program is an added layer to our claims handling process, ensuring the injured worker is included in all communications and decision-making
- Taking time to hear the injured worker’s fears and questions is our solution.
- Sounds simple, but the results are significant: faster healing and claims resolution, and lower litigation and claims costs.
Arrowhead Workers’ Compensation Program, through our claims administrator American Claims Management, has added Claims Advocacy as a new – and important layer of the claims handling process, ensuring that the injured worker’s voice is genuinely heard.
New steps in our claims process ensure we defend and safeguard the injured worker’s rights, genuinely considering their concerns and wishes when we make decisions about their lives.
This extra layer of empathy and compassion is strictly for the injured worker, where our claim administrator’s customer service representatives, adjusters and field nurses – everyone who touches the claim – take extra time to hear the worker’s views and concerns, answering every question and calming their fears.
Sounds simple, doesn’t it? Ensuring that an injured worker is genuinely heard and taking time to answer all questions reassuringly. But Claims Advocacy is bringing about significant results.
Related: How effective is your client’s return-to-work program?
What does Claims Advocacy include?
Here’s what we include in our Claims Advocacy program:
- Claim Contacts. We’re helping the injured through the claim process, making them a part of their recovery, not sitting on the sidelines.
- Dedicated RTW Program. Working with the employer, injured and treating physician to help the injured return to work safely.
- Head Injury Program. Ensuring treatment is provided according to evidence-based guidelines, improving return-to-work outcomes and reducing disability duration.
- Pre-Surgery Pain Screening Program. Preparing the injured for what is to come, addressing concerns before the procedure.
- Utilization Review Surgery Denial Review. Ensuring the injured understands a denied procedure and what the next steps are; working with the requesting physician to ensure the best treatment is provided.
- Rapid Response. Early intervention to proactively address high risk claims, to produce better medical outcomes. The program includes triggers to escalate the claims handling process when any of these are present:
-
- Head injury
- Employee reports injury happened while at lunch, going to and from work, or driving in company vehicle
- Late Report over 30 days
- Repetitive Motion or Cumulative Trauma
- Traumatic Event/PTSD
- Any claim with potential compensability concerns
We’ve found that slowing down, patiently listening to the injured worker and following the advocacy protocol help us resolve claims faster with less litigation and lower payouts, because the patient observes that the insurance company is working WITH them, rather than AGAINST them.
Related: Avoid these top 7 workers’ compensation claim mistakes
Claims Advocacy successes
Take a look at our success:
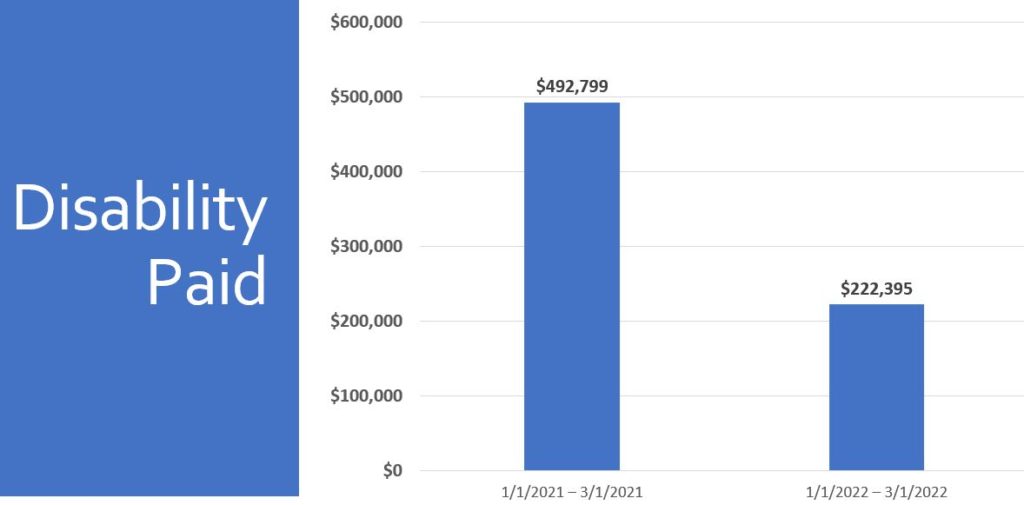
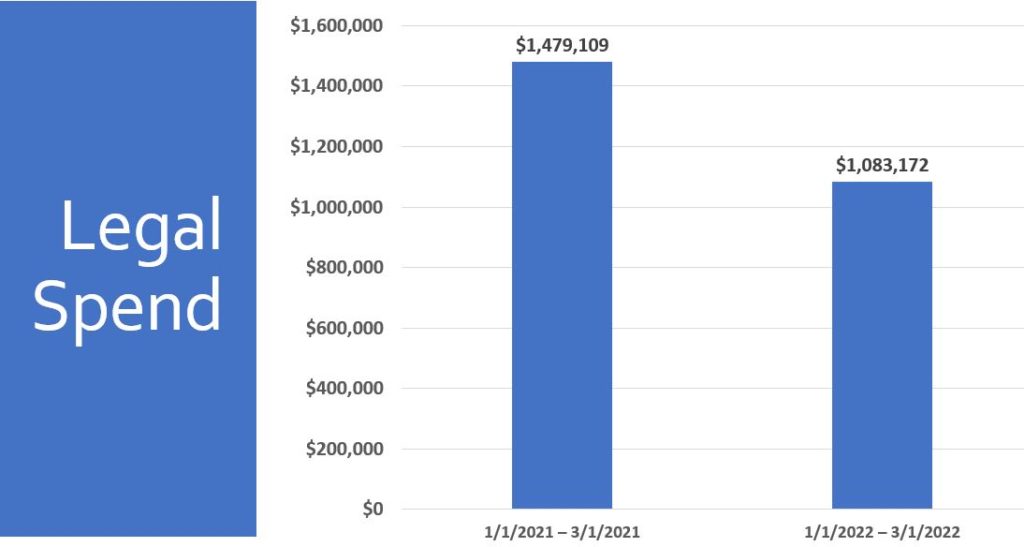
Lower litigation rates and faster returns to work are some of the positive results that stem from our claims advocacy approach.
Related: How faster workers’ compensation claim reporting can reduce costs
Case study
We’re helping the injured through the claim process, making them a part of their recovery, not sitting on the sidelines. Here’s a quick case study:
A worker’s injury was greatly complicated by his poorly controlled diabetes; meanwhile, his employer questioned whether this was a new injury. Our investigation showed that it was indeed a new injury. Initial prognosis showed a high probability of losing his foot.
The adjuster kept in contact with injured worker and field case manager, to ensure that all medical treatment and transportation were provided.
Through advocacy intervention we were able to save his foot and resolve the complex medical treatment. The injured worker was released to full duty and discharged from care. All future exposure was eliminated.
It’s a simple concept that brings tremendous results: Faster healing. Speedier claims resolution. Reduced claims costs.
Agents, take a look at our Workers’ Compensation Program to add to your portfolio of insurance solutions.

